Clinical Trial and Human Research Rules for NIH Proposals
Some years ago, NIH revised their classification of what research is considered a clinical trial. Key definitions and related grant preparation items changed in January 2017. If it’s been a while since you submitted a grant or you’re moving into human subjects research, read on for details, as well as some good side effects of the current forms.
Definitions of Clinical Trials

This might be a clinical trial.
If you work with human subjects, NIH may now consider your research a clinical trial. Their guidance is to ask yourself these questions:
- Am I working with human subjects? (If you are working purely with extant human data or specimens, but not with actual human subjects, you would answer no to this question.)
- Am I prospectively assigning humans (or providing access) to an intervention, such as a drug, device, or activities designed to change behavior? (I.e., you are not studying the effects of someone else’s completed intervention.) Change in criteria alert: You would say yes even if you’re assigning everyone in your study to receive the intervention. The term “trial” no longer implies randomized exposures with a comparison group.
- Is your study designed to evaluate the effect of that intervention?
- Is that effect a health-related biomedical or behavioral outcome?
If you answered “no” to any of these, you are not doing a clinical trial. If you answered “yes” to all of them, congratulations, you are now a clinical trialist. You can also use NIH’s nifty decision tool to double check if your research is considered a clinical trial.
Still not sure? Visit their extensive list of case studies to find studies analogous to your work described and defined. Especially if you are doing observational studies, which can be particularly tricky to classify, NIH advises you to contact your program officer should your research fall into a gray area that could be a clinical trial but maybe isn’t.
Different RFAs exist for proposals that will involve one or more clinical trials and proposals that won’t, or some institutes are keeping the same RFA for both trial and non-trial proposals and calling it “clinical trial optional.”
This includes K awards. K’s have been divided into “clinical trial required” and “independent clinical trial not allowed.” Here’s some relevant language from a K01 RFA:
Independent Clinical Trial Required
This Funding Opportunity Announcement (FOA) is designed specifically for candidates proposing to serve as the lead investigator of an independent clinical trial, a clinical trial feasibility study, or a separate ancillary clinical trial, as part of their research and career development. (PA-20-176).
Independent Clinical Trials Not Allowed
This Funding Opportunity Announcement (FOA) is designed specifically for applicants proposing research that does not involve leading an independent clinical trial, a clinical trial feasibility study, or a separate ancillary clinical trial. Applicants to this FOA are permitted to propose research experience in a clinical trial led by a mentor or co-mentor. (PA-20-190)
If you’re writing a K and doing a clinical trial as it is now defined, your reviewers will also be judging it on additional trial-related criteria, such as whether you show you have the ability to implement your clinical trial, as well as whether you have or plan to get the training necessary in data management and statistics relevant to performing your trial. In addition, they will consider if your mentors are qualified to train you in performing this trial, and whether your study is feasible, reasonable, and well-designed. They will also review your study timeline. (Reviewers have been considering these features all along, and now many of the criteria are explicitly examined.)
PHS Subjects and Clinical Trials Information Form
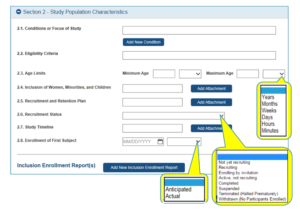
Some parts of the new form ask you to put in simple information via dropdowns rather than attachments.
The PHS Human Subjects and Clinical Trials Information Form is more streamlined and includes items previously scattered across multiple parts of the typical grant proposal, but it does require several different attachments you’ll need to write, up to 12 depending on the type of trial you’re doing.
Forms-F instructions from NIH provide guidance on how to fill out the form and what to write in attachments, including the study timeline and dissemination plan. If your proposal includes multiple studies, each study you’re planning may require copies of these attachments. Here are a few examples:
Recruitment and Retention Plan
Describe how you will recruit and retain participants in your study. You should address both planned recruitment activities as well as proposed engagement strategies for retention.
Study Timeline
Provide a description or diagram describing the study timeline. The timeline should be general (e.g., “one year after notice of award”), and should not include specific dates. Note: Additional milestones or timelines may be requested as just-in-time information or postaward.
Dissemination Plan
Explain briefly your plan for the dissemination of NIH- funded clinical trial information and address how the expectations of the policy will be met. The plan must contain sufficient information to assure the following:
-
the applicant will ensure that clinical trial (s) under the award are registered and results information is submitted to ClinicalTrials.gov as outlined in the policy and according to the specific timelines stated in the policy;
-
informed consent documents for the clinical trial (s) will include a specific statement relating to posting of clinical trial information at ClinicalTrials.gov; and
-
the recipient institution has an internal policy in place to ensure that clinical trials registration and results reporting occur in compliance with policy requirements.
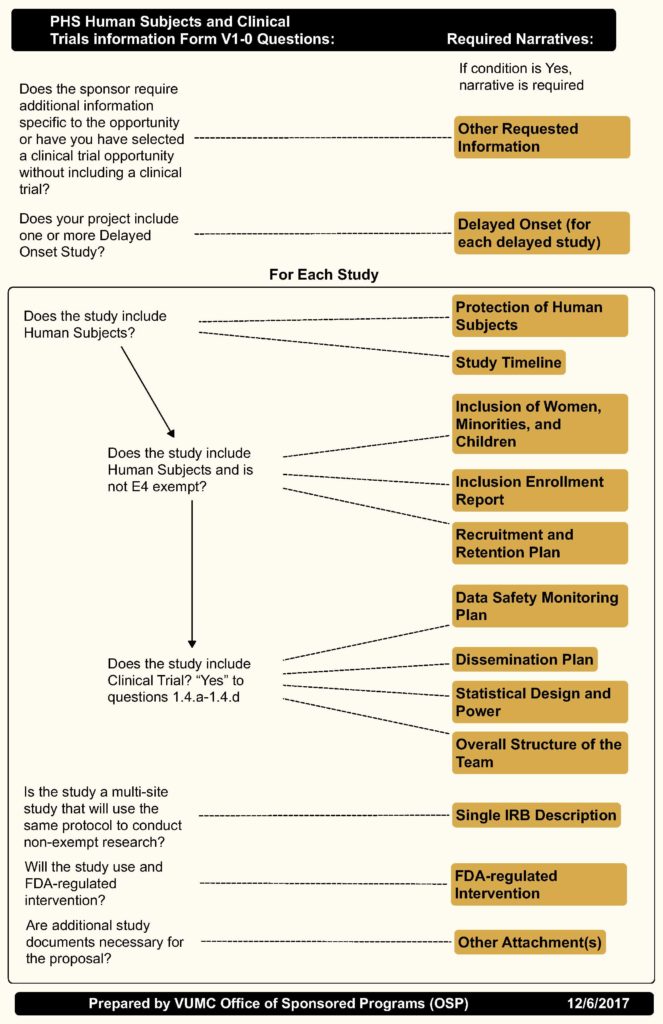
The fillable forms you can find by starting a grant in ASSIST or by using your institution’s grant submission software ask you a few questions to begin and then use branching logic to help you figure out which attachments to include. Shane Crounse at Vanderbilt has also created an infographic that helps you decide what you need to start writing before you get to the submission stage.
This nine-minute video tutorial is worth the investment of time as it walks you logically through the current set of forms. It’s also worth taking a look at the annotated version of the new forms for further clarification.
If you aren’t doing a clinical trial, you’re not entirely off the hook. You need to explain why your application doesn’t involve human subjects research, but after that you’re done with this form.
But What About My Approach?!
Good news: Although you’re required to present the information in these attachments in a different way, the attachments are largely made up of what you used to put in the Approach section. As an exercise, Shane noted he was able to get all the information he needed for the form just by pulling it from the text of a funded grant in the old format.
Bad news: NIH frowns on copying and pasting between the approach and the attachments. Instead, they ask you to refer between the two. Our suggestion to keep reviewers from having to flip around a 70-page PDF (and then tear their hair out in frustration) is to briefly describe crucial elements of recruitment, enrollment, and other human subjects materials in your approach and note that details can be found in the Human Subjects and Clinical Trials Information Form.
Why Modify Forms?
Why did NIH do this? To increase transparency and accountability. By pulling out human subjects and associated trial information in uniform formats, NIH stats wonks will know instantly how many PIs are conducting trials or working with participants, what they’re doing, when they’re doing it, and to whom, rather than hunting through long research plans. Ultimately, we’ll get some interesting data out of this.
Good News: More Space for Your Science
We’ve saved the best for last. Moving so much of the human subjects information to a different form frees up a lot of space in the 12 pages you still have for your research strategy. You now have more room to tell reviewers about your cool science. That can’t be all bad.
Home Page ImageCreator: Vanderbilt University
Source: https://www.flickr.com/photos/digitalvu/5515731056/





2 Comments